So now coconut oil is bad for me??? (*Scratches head*)

You may have seen headlines the past couple weeks that the American Heart Association is making claims against saturated fat, LDL, and heart disease. In the Dietary Fats and Cardiovascular Disease Advisory put out by the AHA, they reviewed research on a variety of different oils and are making recommendations against coconut oil.
The AHA is saying that “coconut oil raises ‘bad’ cholesterol in the same way as other foods high in saturated fats like butter and beef” and they are advising against the use of coconut oil "because coconut oil increases LDL cholesterol, a cause of CVD [cardiovascular disease], and has no known offsetting favorable effects." In other words, the AHA is recommending that you replace saturated fat (specifically coconut oil) with polyunsaturated (like Omega 6 and Omega 3) and monounsaturated fat (like avocados), without reducing the total amount of fat you eat, to lower your risk of developing cardiovascular disease.
Let’s remember that the media has a habit of using trends to write eye-catching headlines that may or may not be rooted in scientific evidence. But before we make any decisions related to headlines, let’s get informed and know the science for ourselves.
What is coconut oil?
Coconut oil is oil derived from coconuts that is mostly made up of medium-chain triglycerides. MCTs are triglycerides and fatty acids with a 6-12 carbon length chain. Coconut oil is 90% saturated fats and about 65% are mostly from medium chain fatty acids. Most studies and articles that discuss the health benefits of coconut oil are actually discussing the health benefits of medium-chain triglycerides, not coconut oil specifically.
- MCTs are small and can permeate cell the cell membrane easily.
- MCTs are digested easily, without putting extra strain on your digestive system.
- MCTs are sent directly to the liver and can be used for energy instead of being stored as extra body fat.
- MCTs are “designer” fats with varieties used often in high fat, low carb diets and special varieties used in “bulletproof” or fat filled coffees, boasting improved brain function.
The Complex World of Lipids
It’s true, saturated fats can increase both your LDL and HDL levels. It is also true that saturated fat positively impacts the ratio of LDL and HDL (we will get into that a little later.) What you don’t get from the AHA’s advisory report, is information on LDL particle size or number. Without those pieces of information, you don’t have a comprehensive picture of your cholesterol and heart health. But let’s start with the big picture and take a look at what fat really is.

Source: Christa Biegler, R.D.

Source: Alfaro, D. (2014, December 19). Know Your Fats: The Good, the Bad, and the Ugly. Retrieved June 23, 2017, from https://www.thespruce.com/all-about-fats-995463 and Jill Rohlfs.
A fat is not just fat. There are triglycerides, phospholipids, and sterols.
- Triglycerides are the major source of fat in the diet as well as the major storage form of fat in the body.
- Phospholipids such as lecithin, are constitutes of the cell membrane. Phospholipids are both water- and fat-soluble, which means they can help fat-soluble substances like vitamins and hormones pass effortlessly in and out of cells.
- Sterols are important compounds in the body such as bile acids, sex hormones, adrenal hormones, vitamin D, and cholesterol. Interestingly enough, cholesterol can make bile acids, steroid hormones, and vitamin D.
More about Cholesterol

Our bodies need cholesterol. Each cell is surrounded by a cell membrane that has a “lipid bilayer.” Cholesterol is one of the major components that make up this lipid bilayer. The cell membrane’s lipid bilayer has a HUGE responsibility: to control how the cell moves, interacts with other cells, and transports things in and out of the cell.
Almost every cell in the body can produce its own cholesterol and doesn’t require the consumption and delivery of extra cholesterol. Cholesterol can be separated into two categories: endogenous and exogenous cholesterol.

- Endogenous cholesterol: cholesterol made in the body.
- Your liver manufactures cholesterol (800-1500 mg/day) from carbohydrates, fats, and proteins. Because of this, you do not need to consume cholesterol from your food.
- Exogenous cholesterol: cholesterol from outside the body (from foods)
- Cholesterol only becomes harmful when it contributes to the formation of plaque in the artery walls and ultimately the development of atherosclerosis and an increased risk of a heart attack or stroke.
Is Cholesterol good or bad?
- According to Dr. Peter Attia, all cholesterol is good: “The only “bad” outcome is when cholesterol ends up inside of the wall of an artery, most famously the inside of a coronary artery or a carotid artery, AND leads to an inflammatory cascade which results in the obstruction of that artery (make sure you check out the pictures in the links, above). When one measures cholesterol in the blood – we really do not know the final destination of those cholesterol molecules!”
How does cholesterol maneuver through the body?
Cholesterol is not soluble in water. Because of this, cholesterol needs to be transported by lipoproteins. Lipoproteins (see descriptions below) are clusters of lipids associated with proteins that serve as transport vehicles for lipids in the lymph and blood.
- Chylomicrons are the largest and least dense of the lipoproteins. They transport diet-derived lipids, mostly triglycerides, from the intestinal cells to the rest of the body via the lymph system.
- VLDL (Very-Low Density Lipoproteins) are the type of lipoprotein made by the liver to transport lipids to various tissues in the body.
- LDL (Low Density Lipoproteins) are the type of lipoproteins derived from VLDL as triglycerides are removed and broken down.
- HDL (High Density Lipoproteins) are the type of lipoprotein that transports cholesterol back to the liver from the cells.
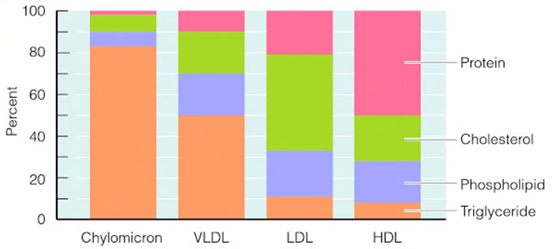
Source: Understanding Normal and Clinical Nutrition
What about particle size?
Most medical professionals focus on LDL as a way to predict heart attack risk, regardless of the fact that many people with heart disease do not have especially high LDL levels. This is because some LDL particles are smaller and some are larger.
Particle size and amount are not regularly tested for to indicate a risk for heart disease, but they should be because smaller LDL particles can pack together and easily get into arteries. On the other hand, larger LDL particles might be less dangerous because they cannot get into the arteries as easily.
What does the research say about MCTs and coconut oil?
- Some studies claim that replacing calories with MCTs (like coconut oil) can result in a small increase in the rate of fat loss over time, as long as you do not exceed your daily caloric requirement.
- Not only can incorporating MCTs in your diet impact the rate of fat loss, but it may also temporarily increase your metabolic rate and the speed at which fats are broken down in the body. This effect has been shown to be temporary and may only last for the first two weeks of incorporating coconut oil into your diet.
- MCTs (like coconut oil) create more ketone bodies than longer chain fatty acids.
- When eating a low carb diet (typically less than 50g carbohydrates/day), insulin levels go down and fatty acids are released from your body’s fat stores. Once the fatty acids are released, most of them are transferred to the liver and become ketone bodies. While fatty acids cannot be used for energy in the body, ketones (ketone bodies) can be used for energy in the absence of glucose because they can cross the blood-brain barrier.
Incorporating coconut oil alone into your diet is unlikely to create a noticeable difference in fat loss, but replacing other dietary fats in your diet with MCTs like coconut oil may support your fat loss goal.
Should you replace saturated fats with polyunsaturated and monounsaturated fats?
The AHA’s recommendation to replace saturated fat with polyunsaturated fats (without specifying type and ratio) and monounsaturated fats may be flawed.
The typical American diet consists of an excess of omega-6 polyunsaturated fatty acids like vegetable oils, some articles showing as much as a 16:1 ratio of Omega 6 to Omega 3.
The AHA currently recommends that in order to reduce the risk of heart disease, saturated fats should be replaced with polyunsaturated fats, without specifying which type of polyunsaturated fatty acid (PUFA)--Omega 3 or Omega 6. Linoleic acid Omega 6s can be elongated to arachidonic acid and ultimately made into pro-inflammatory compounds. These pro-inflammatory compounds may increase the risk of heart disease when consumed excessively as they typically are now.
Omega 6s are still an important PUFA and become less inflammatory when the quality is considered and Omega 3s are consumed more frequently to bring the ratio closer to 4:1.
Replacing saturated fats with monounsaturated fatty acids, like avocado and olive oil, is associated with reduced risk of cardiovascular disease. According to a recent study that reviewed studies over the last three years for cardiovascular risk factors, replacing saturated fat with monounsaturated fatty acids decreases a variety of CVD related risk factors such as: total cholesterol, LDL-cholesterol, LDL to HDL cholesterol ratio, and LDL particle number.
What about genetics?
The body’s response to saturated fat is bio-individual. A very interesting gene, APOA2, has demonstrated that there is a connection between different genotypes and an individual’s response to saturated fat. APOA2 has three variations: GG, AG, and AA.
According to scientific research of Dr. Nathan West, people with the GG variation have been found to have a higher BMI if consuming more than 22g of saturated fat each day and should consider restricting their consumption of saturated fat to less than 22 g per day. Those with the AG or AA variation of APOA2 may not need to restrict their consumption of saturated fat.
According to this study, regardless of the variation of APOA2 (GG, AG, or AA), individuals that consume less than 22 g of saturated fat per day did not have an increased BMI. In other words, this gene comes into play when saturated fat intake is high, but not when it is low.
What does 22 g of saturated fat look like? See how much saturated fat is in your food based on the USDA database.
So what does all of this mean to me?
This is going to be shocking, I know, but here it goes…..it depends on the individual.
Bottom line: The blanket statement from the AHA doesn’t apply to everyone.
---> Depending on your genetics (if you have the APO gene), too much saturated fat (of which coconut oil is one of the only plant sources) could make your lipid panel wonky. Pssstttttt…..we can do a genetic test so you know the valuable information related how your body can and cannot process different nutrients; there are times where it could literally be lifesaving. Email: [email protected]
---> For the rest? It might be just fine. Nutrition is constantly evolving and changing and we should keep an open mind. However, a less processed, plant based diet (i.e. has a plant based source of saturated fat) is generally very healthful and the MCT oils in coconut oils have shown benefit when used properly. Not to mention other beneficial compounds in coconut oil like caprylic acid, which boasts antifungal and other benefits.
----> Variety is key. Most people are getting an undesirable ratio of unsaturated fatty acids--the Omega 3s vs Omega 6s (see the flowchart near the top for context). They are getting too many Omega 6s, like sunflower and vegetable oils that are pervasive in processed foods and not enough Omega 3s like fatty fish, flax and chia seeds. While we need both, it’s proinflammatory when our ratios are heavily skewed from the desired 4:1 to a 16:1. Coconut oil might be another less inflammatory oil for most with it’s unique shorter chain triglycerides, making it more digestible.
How do we do it? Eat more whole, unprocessed foods, wild caught meats, and use foods in their most natural form possible as much as possible.
The old saying “K.I.S.S.” saying rings true, Keep It Simple Silly.
Be informed, remember we all respond differently to different nutrients (which is why a genetic test is a good, one time information panel) and stay objective for both sides.
This article does not take the place of tailored advice from your healthcare professional. See the disclaimer in the footer below for more information.
If you are looking for a tour guide to help you navigate cutting edge nutrition, gut healing, or you want to explore your own genetics or functional testing please email me at [email protected].
Images created from original data sources. For image use, please link to this article.
Sources
Attia, P. (2012, June 17). The Straight Dope on Cholesterol Pt. 1. Retrieved June 25, 2017, from http://eatingacademy.com/nutrition/the-straight-dope-on-cholesterol-part-i
Alfaro, D. (2014, December 19). Know Your Fats: The Good, the Bad, and the Ugly. Retrieved June 23, 2017, from https://www.thespruce.com/all-about-fats-995463
Corella, D., Peloso, G., Arnett, D. K., Demissie, S., Cupples, L. A., Tucker, K., … Ordovas, J. M. (2009). APOA2, Dietary Fat and Body Mass Index: Replication of a Gene-Diet Interaction in Three Independent Populations. Archives of Internal Medicine, 169(20), 1897–1906. http://doi.org/10.1001/archinternmed.2009.343
Dietary Guidelines for Americans 2015–2020 8th Edition. (n.d.). Retrieved June 25, 2017, from https://health.gov/dietaryguidelines/2015/guidelines/
Examine. (2017, June 23). 21 of the best arguments for and against coconut oil. Retrieved June 23, 2017, from https://examine.com/nutrition/21-of-the-best-arguments-for-and-against-coconut-oil/?utm_source=newsletter&utm_medium=email&utm_campaign=blog-062217
Examine. (2017, June 21). Coconut Oil - Scientific Review on Usage, Dosage, Side Effects. Retrieved June 23, 2017, from https://examine.com/supplements/coconut-oil/
Gunnars, K. (2017, June 04). How to Optimize Your Omega-6 to Omega-3 Ratio. Retrieved June 27, 2017, from https://authoritynutrition.com/optimize-omega-6-omega-3-ratio/
Joris, P. J., & Mensink, R. P. (2016). Role of cis-Monounsaturated Fatty Acids in the Prevention of Coronary Heart Disease. Current Atherosclerosis Reports,18(7). doi:10.1007/s11883-016-0597-y
Le Vere, A. (2015, July 02). In Defense of Coconut Oil: Rebuttal to USA Today. Retrieved June 23, 2017, from http://www.greenmedinfo.com/blog/defense-coconut-oil-rebuttal-usa-today
May, A. (2017, June 16). Coconut oil isn't healthy. It's never been healthy. Retrieved June 23, 2017, from https://www.usatoday.com/story/news/nation-now/2017/06/16/coconut-oil-isnt-healthy-its-never-been-healthy/402719001/
Mercola, J. (n.d.). The Truth About Saturated Fats and The Coconut Oil Benefits. Retrieved June 23, 2017, from http://articles.mercola.com/sites/articles/archive/2010/10/22/coconut-oil-and-saturated-fats-can-make-you-healthy.aspx
Palsdottir, H. (2017, June 03). What is Ketosis, and is it Healthy? Retrieved June 23, 2017, from https://authoritynutrition.com/what-is-ketosis/
Rapaport, L. (2017, June 20). Coconut oil has more 'bad' fat than beef and butter, heart doctors warn. Retrieved June 23, 2017, from https://www.theglobeandmail.com/life/health-and-fitness/health/coconut-oil-has-more-bad-fat-than-beef-and-butter-heart-doctors/article35392172/
Rolfes, S. R., Pinna, K., & Whitney, E. N. (2012). Understanding normal & clinical nutrition. Boston, MA: Cengage Learning.
Sacks, F. M., Lichtenstein, A. H., Wu, J. H., Appel, L. J., Creager, M. A., Kris-Etherton, P. M., . . . Horn, L. V. (2017). Dietary Fats and Cardiovascular Disease: A Presidential Advisory From the American Heart Association. Circulation. doi:10.1161/cir.0000000000000510
Should you seek advanced cholesterol testing? (2014, May). Retrieved June 25, 2017, from http://www.health.harvard.edu/womens-health/should-you-seek-advanced-cholesterol-testing-
Do you need a detox?
Getting "too old" to handle alcohol?
Sensitive to smells or metals?
Skin issues?
Detox isn't just juice cleanses & snake oils. It's a process that our body is trying to do all day long.
Take the quiz to find out if it's time for a detox.





